A Guide to Breast Cancer in Older Adults
Updated on: October 2022
Reviewed by: Nancy Leahy, RN, APNP

Breast cancer is the most common form of cancer found in elderly women. A woman has a one-in-eight chance of developing breast cancer over her lifetime, according to the National Cancer Institute. The older a woman is, the more likely it is she will be diagnosed with the disease. On average and across all races, there is about a 9 percent chance that a 60-year-old woman develops senior breast cancer over her next 20 years.
Nearly 275,000 new cases of breast cancer are diagnosed every year, with more than three million survivors of the disease living at any given time, according to the American Cancer Society. About half of the newly diagnosed breast cancer cases come from women over the age of 60, and another 20 percent come from women over 70 years old. At age 80, the chances of you developing breast cancer over the rest of your life begin to decrease, according to Harvard Medical School.
Unfortunately, women over 65 who are diagnosed with early onset breast cancer are more likely to pass away due to the disease. Women in that same age group are more likely to have the cancer recur, as well. More than 40,000 women die from breast cancer every year.
It’s vital that women—and their loved ones—know the warning signs, causes, and different types of breast cancer, as well as how and when to get tested, and how it can be treated and prevented.
Find What You Need
Types of Breast Cancer
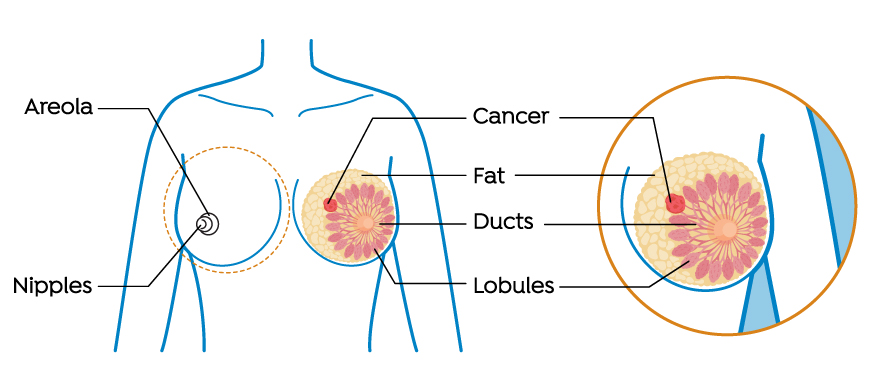
Breast cancer is a blanket term for any form of cancer that develops in and around the breast, such as the lobule (the part of the breast that makes milk), the milk ducts (these carry the milk around the breast), though there are specific forms of the cancer that affect different parts of the breast. Generally speaking, breast cancer is either:
- Invasive: The cancer spreads to healthy tissue.
- Non-invasive: The cancer is localized to the milk ducts and cells of the breast.
One of the most common form of breast cancer is invasive ductal carcinoma (IDC). This form of breast cancer starts in the milk ducts and moves to other healthy tissue. There is a non-invasive form of this type of cancer that starts in the milk ducts, too, but BreastCancer.org notes that most breast cancers are invasive.
Other important forms of senior breast cancer include the following:
Invasive Lobular Carcinoma:
Similar to IDC, this form of cancer can spread to other parts of the breast, but it starts in the lobules. There is a non-invasive form, too, meaning the cancer stays in the lobule where it started.
Inflammatory Breast Cancer:
This is a rare form of breast cancer that makes up about 1 percent of all cases. It starts with a reddening and inflamed breast and then spreads quickly to surrounding tissue such as the lymph nodes. Within a few days or a week, it can spread from the breast to other areas.
Paget’s Disease:
This is a rare form of cancer that affects the nipple. It starts in or just behind the nipple and can spread to other parts of the breast.
Angiosarcoma:
While this is an overarching term for any form of cancer that affects the blood and lymph vessels in your body, it can occur in the breast, though it’s rare.
Any of these cancers can recur, even if treated in the early stages. The cancer may recur in the same spot as before or in a different area if leftover cells survived after the cancer previously spread.
There is also a form of breast cancer that occurs in men, but it makes up less than 1 percent of all related cases. If a man does develop breast cancer, it almost always starts in the undeveloped milk ducts.
Women are 126 times more likely to be diagnosed and die due to breast cancer than men.
Causes of Breast Cancer
Breast cancer is caused by a mutation of cells in the breast, but it’s not exactly clear what causes that mutation. Whereas with lung cancer, for example, it’s easier to point to an activity like smoking as the root cause, the same does not hold true for breast cancer.
However, there are risk factors for senior breast cancer and they include:
It should be noted that these risk factors are not direct causes of breast cancer.

Gender:
Breast cancer occurs almost exclusively in women. More than 99 percent of breast cancer cases happen in women.

Age:
The older you get, the more likely it is you will develop breast cancer. However, once you reach 75 years old, the chances of getting breast cancer over the remainder of your life starts to decrease.

Genetics:
The American Cancer Society says that about 5 to 10 percent of all breast cancer cases are inherited. The mutated genes most likely to be passed on that indicate a higher likelihood of having cancer are BRCA1 and BRCA2. You have about a 70 percent chance of getting breast cancer by 80 if you have one of these gene mutations. Men with the BRCA2 mutation have a higher risk of developing breast cancer than men without it, too.

Previously having Breast Cancer:
If you’ve had breast cancer in the past, you’re more likely to get it again.

Race:
White and African-American women have higher rates of breast cancer.
Dense Breast:
Dense breast tissue can be a risk factor for breast cancer. Dense breasts have more glandular and fibrous tissue than they do fatty tissue.
Family History:
If a close family member such as your mom, sister, or grandmother have had breast cancer, your chances of getting the disease are higher.

Reproductive History:
If you started your period before age 12 or started menopause after age 55, you are more likely to get breast cancer. Women who have never been pregnant have a higher risk as well.
Signs and Symptoms of Breast Cancer
One of the most important steps in beating breast cancer is catching it at the earliest possible stage. This is why it’s vital to know the signs and symptoms of senior breast cancer.
The most common symptom is a lump on your breast. While most lumps on the breast are benign, about 20 percent are cancerous. They’re especially concerning if you’re over 40, because it is more likely the lumps are connected to cancer rather than an injection or benign tumors. The root cause of the lump is often seen during mammograms before they develop into lumps on the breast. So while lumps can be a sign, there are other signs on and around the breast that can indicate the presence of senior breast cancer. These include:

Lump on the Breast:
The most common symptom is a lump forming on the breasts. While 20% of lumps are cancerous, the risk increases with age.

Discharge from the Nipple:
Any sort of nipple discharge, whether it’s clear or discolored, runny or thick, can be an indication of breast cancer. However, the cause can also be a side effect of other medical issues or from breastfeeding, especially if it’s a milky color.

Swelling and Soreness:
Breast cancer can cause a general swelling or soreness of your breasts. The swelling would be significant enough to change the size of the breast that is effected, even if one is already a different size than the other. The swelling can affect the whole breast or a part of it, and it can change the overall size and shape of the breast.

Nipple Inversion:
The composition of your nipple can change based on the presence of breast cancer. The cancer cells can affect the area right behind your nipple, causing it to turn inward or start inverting.

Redness of the Skin:
One of the primary effects breast cancer has on the skin is a general redness, especially in the area where the cancer cells are affecting the lymph nodes. This can be one confined area or across the whole breast(s)

Skin Dimpling:
This occurs when parts of the skin on the breast invert and create a small dimple. Like the inversion of the nipple, this can show where the cancer is present. These dimples can also indicate that the cancer is aggressive.

Swelling in the Underarm:
The first place cancerous cells usually travel after affecting the breast is to the lymph nodes in the under arm. Swelling or tenderness in the region can suggest breast cancer is present and has spread.
Other Changes to the Skin:
In addition to redness, swelling, and dimpling, breast cancer can reveal itself through peeling, flakiness, and crustiness in the area surrounding the areola and other areas of the breast.
How to Get Screened for Breast Cancer
If you notice you’ve experienced some of the symptoms of senior breast cancer, visit the doctor as soon as possible. Not next week, not next month. As soon as the doctor can fit you in. When making the appointment, you should note you the symptoms you have experienced. You should also get a yearly test even if you aren’t showing any symptoms.
Your doctor will perform a handful of tests to determine if your symptoms are the result of the presence of cancer in your breasts. Some of these tests include:
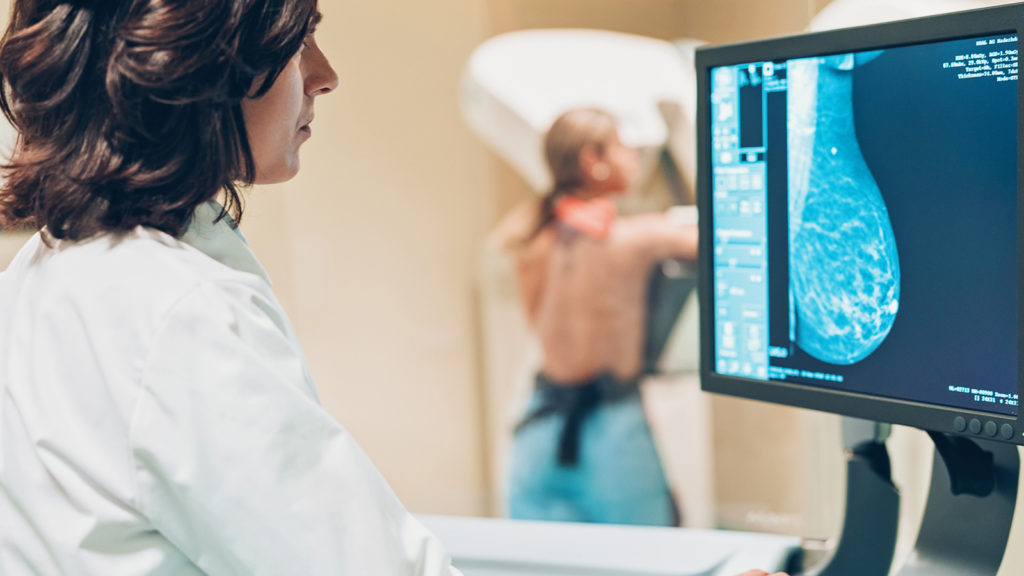
Mammogram
A mammogram is an X-ray of the breast(s). The process starts with you standing in front of an X-ray machine and placing your breast on a clear plate. The machine then moves another clear plate on top of your breast, which is flattened with a little bit of pressure. This process can be uncomfortable and sometimes even painful, but it will only take a few seconds once the breast is in the right place. The machine takes photos of both breasts from the front and from the side.
The Centers for Disease Control and Prevention (CDC) suggest that you avoid wearing deodorant, perfume, or any powder the day of the exam as they can alter the image and raise false flags. They also suggest avoid wearing a dress to the exam, and that you schedule the exam at a time when you aren’t on your period, during which your breasts can swell and be tender.
There are no strict guidelines for when a woman should start receiving a yearly mammogram, though it’s recommended that yearly exams start at age 45. They can move to every two years when you reach 50 to 55 years old. When you turn 75, there aren’t any guidelines for a yearly or every-other-year mammogram, and getting a screening at that point is up to you and your doctor’s discretion. You may want to start getting mammograms earlier than 45 if you have a family history of breast cancer, though that is of course up to you. If you’re unsure when you should start, consult your primary care physician.
Biopsy
This type of exam is performed to confirm a breast cancer diagnosis. It’s usually the step that follows all of the other types of exams when a doctor notices something that may be breast cancer.
During a biopsy, a doctor will extract cells from the area he or she believes the cancer is in your breast with the help of a needle and an X-ray. The cells will then be tested for cancer at a lab, which will either confirm or disprove the diagnosis. If confirmed, the test results will show if the cancer is invasive or non-invasive and how far along the cancer has developed, according to the Mayo Clinic.
Breast Exam
This is a physical exam done by a doctor, who will feel for any lumps, bumps, dimples, skin deformities, or other problems. He or she will also feel around the lymph nodes of your armpits, which is typically the first area that invasive cancer spreads to outside of the breast. Breast exams are suggested for adult women before age 40. They are typically done in conjunction with mammograms.
Ultrasound and MRI
Ultrasounds and MRIs are exams that help get a deeper image of the breast. Ultrasounds use soundwaves to depict clearer images of a lump on and inside the breast, while MRIs use radio waves to accomplish a similar task. Neither of these tests use radiation.
Breast Cancer Treatment and Prevention
Once a breast cancer diagnosis is confirmed, treatment starts almost immediately. Treatment depends on the type of cancer, the stage it is in, the size of the tumor is and if it has spread, and the type of tumor. All of this information helps doctors determine how to best move forward in your treatment.
Treatment options for senior breast cancer include:
Mastectomy:
This is surgery that removes the whole breast that is affected by the cancer. There are different kinds of mastectomies where the removal of tissue will move up to the lymph nodes in the armpit area. If the cancer has spread to the muscles behind the chest wall, surgeons may remove that, too. If cancer is present in both breasts, the surgery is known as a double mastectomy. Some people will have a mastectomy if it’s believed there is a high chance they will contract the disease due to family history.
LUMPECTOMY:
This is another form of surgery on the breast – it’s a partial removal of breast tissue. It’s typically done on patients with less invasive forms of breast cancer in their earlier stages. The goal of a lumpectomy is to remove all the cancerous tissue while making sure the breast looks the same as before.
Treatment depends on the type of cancer, the stage it is in, the size of the tumor is and if it has spread, and the type of tumor.
Chemotherapy:
Chemotherapy drugs and treatments are meant to attack and kill cancer cells. It can be administered intravenously, with a pill, through an injection, with a cream, and other ways. The most common side effects include nausea, fatigue, vomiting, and hair loss.
Radiation:
This form of therapy also aims to attack and kill cancer cells, only this treatment is more localized. Radiation uses high-energy beams to attack the area where the cancer cells are present. It’s often done in conjunction with lumpectomies to make sure the area where the cancer is present receives the full force of treatment. Side effects can include coughing and shortness of breath.
Hormone Therapy:
Two of every three cases of breast cancer are “hormone-receptor positive,” according to the ACA, which means the tumor and cells respond to high levels of hormones in women, particularly estrogen. The high levels of hormones can help the cancer spread. Hormone therapy is a way to balance that. The drugs used for hormone therapy block the hormone receptors on cancer cells to help stop them from growing. They may also lower your hormone levels to help accomplish the same task.
You may also be treated to help manage any pain, eating issues, weight loss, or other physical and mental side effects that arise due to treatment. Not every breast cancer will require the same type of treatment and, ultimately, the choice is up to you what course of action you want to take. Your doctor should discuss all available treatment options, how they will help reduce the presence of the cancer, and how the treatment will help ensure the cancer will not resurface if the treatment is successful.
Unfortunately, there is no clear, defined way to prevent breast cancer. However, there are suggestions made by researchers and doctors in order to reduce the risk of getting breast cancer. According to the CDC, these include:
- Maintaining a healthy weight
- Not smoking
- Limiting alcohol intake to one or fewer drinks per day
- Being physically active
- Breastfeeding (if you have children)
If you have any questions regarding senior breast cancer, contact your primary care physician or get in touch with an oncologist in your area.